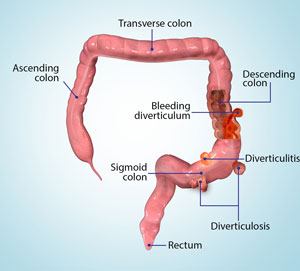
What is Diverticular Colitis?
Diverticular colitis also known as segmental colitis associated with diverticulosis (SCAD) is a condition characterized by chronic inflammation of the mucosa in the sigmoid colon and diverticular disease, a condition in which pockets or pouches develop in the colon wall. Diverticular colitis is restricted to the sigmoid colon and does not affect the rectum.
Causes of Diverticular Colitis
The actual cause of diverticular colitis is unknown, but some of the factors include:
- Mucosal prolapse (shifting or infolding of the mucosal layer)
- Mucosal ischemia (reduced blood supply)
- Subserosal peridiverticulitis and suppurative inflammation (inflammation and pus formation deep in the sigmoid colon wall producing a mass)
- Faecal impaction
- Microbial imbalance in the gut
Symptoms of Diverticular Colitis
Diverticular colitis is most commonly found in men aged above 40 or 50. Some of the common symptoms include:
- Rectal bleeding
- Bloody stools
- Lower left abdominal pain
- Changes in bowel movements such as diarrhoea
- Weight loss
Diagnosis of Diverticular Colitis
Your doctor will review your symptoms and medical history. A physical examination is performed. Diagnostic tests for diverticular colitis include:
- Stool examination: A stool sample is inspected as well as examined in the laboratory for blood.
- Blood test: This test includes evaluating the complete blood count to determine anaemia due to rectal bleeding, infection, and the level of inflammatory biomarkers.
- Flexible sigmoidoscopy: A slender tube with a light and camera at one end is inserted into the last portion of the colon to examine the sigmoid.
- Colonoscopy: A long, flexible tube with a small camera and light source attached to its tip is inserted to examine the large intestine to detect inflammation and ulcers formed in the mucosal lining.
- Biopsy: A small tissue sample (biopsy) from the affected area will be taken and examined under the microscope.
Treatment for Diverticular Colitis
Diverticular colitis is usually self-limiting or easily treated with anti-inflammatory medications. Antibiotics are also usually administered. Blood transfusions may be necessary. The condition usually resolves in a few weeks or months. In rare cases, removal of part of the colon may be recommended. There is usually no recurrence.






